“How do the results of the different methods of bleaching stack up when they are compared? What facts are being considered? How can you know which way is ‘the best’?”
In a previous post, “Whiter Teeth! (Part 2)”, we introduced three procedure strategies for applying bleach to whiten teeth:
- in-office, power bleaching
- at-home, dentist-supervised tray bleaching
- over-the-counter, do-it-yourself bleaching
In our last post, “Whiter Teeth! (Part 3)”, we discussed the importance of analyzing  peer-reviewed scientific research before recommending any procedure or using any material when treating our patients. We want to rely on valid scientific evidence—and not biased opinion—to make objective decisions about what is best for our patients. We quoted two dependable resources [1] [2] that had concluded that at-home, dentist-supervised tray bleaching is best.[3]
peer-reviewed scientific research before recommending any procedure or using any material when treating our patients. We want to rely on valid scientific evidence—and not biased opinion—to make objective decisions about what is best for our patients. We quoted two dependable resources [1] [2] that had concluded that at-home, dentist-supervised tray bleaching is best.[3]
Does that mean that in-office power bleaching is just a hoax? Does that mean that whitening strips from the local pharmacy don’t work? Of course not! But they don’t work as well as at-home tray bleaching.
How do we know? Let’s take an objective approach by listing some scientific facts about getting your teeth whiter. (If you just want a summary conclusion, feel free to jump to the bottom.)
Tooth Whitening Facts
- Each tooth has a maximum whiteness level that it can achieve. It cannot be whitened beyond that maximum level no matter what material or technique is used for bleaching.[4] [5]
- Each tooth has a maximum rate at which the whitening can progress. Once that rate is reached, higher concentrations of bleaching solutions make no difference in the speed of whitening process.[6] [7] [8]
- The eventual whitening result achieved is determined by the properties of each tooth—not the product used.[5] [7] [9] [10]
- Tooth sensitivity is the most common side effect of bleaching.[3] [5] [11]
Bleaching Material Facts
- Although the exact concerntrations from each manufacturer vary a bit, Hydrogen Peroxide (35%) is typically used for in office bleaching while Carbamide Peroxide (10%) is typically used for at-home tray bleaching.
- Tooth sensitivity during treatment is more common with higher concentrations of peroxide bleaching solution.[3] [10]
In-Office Bleaching Facts
- In-office whitening techniques typically utilize a prop to hold the mouth open and isolate the teeth. This process temporarily dries out the teeth. Teeth appear significantly whiter when they are dehydrated. Unfortunately, that whiter appearance reverses completely in a matter of just a few days—sometimes within a few hours—when the teeth become wet with saliva again. [4] [12]
- In-office bleaching procedures usually utilize a bright blue light to “activate” the bleach solution that has been painted on the teeth.
 Several unbiased scientific experiments have compared what happens when half the teeth are whitened with the use of light activation while the other half of the teeth in the same patients were treated without light activation. The light made no difference. [8] [13] [14] Although the teeth were much whiter immediately after treatment, the effect is due to dehydration [15]—not light activation—and reverses in just a matter of days.[11]
Several unbiased scientific experiments have compared what happens when half the teeth are whitened with the use of light activation while the other half of the teeth in the same patients were treated without light activation. The light made no difference. [8] [13] [14] Although the teeth were much whiter immediately after treatment, the effect is due to dehydration [15]—not light activation—and reverses in just a matter of days.[11] - The results from one in-office bleaching treatment are not as white or as long lasting as the outcome from at-home tray bleaching.[4] Satisfaction surveys have shown that patients require 3-4 in-office treatments to achieve the same whitening effect as at-home tray procedures.[11] [16]
- Manufacturers of in-office light-activated power bleaching systems often recommend the use of additional at-home tray whitening to “complete the bleaching process”.[11]
Over-the-counter (OTC) Bleaching Facts
- OTC whitening strips use a “one-size-fits-all” rectangular membrane loaded with bleaching solution. The membrane is pressed against and adapted to the teeth. [3]
- Since the OTC strips are not custom fit for each patient, they can inadvertently be positioned too far over the gums resulting in increased irritation and sensitivity.
- Since the OTC strips are arbitrary in length, it can sometimes be difficult for patients to achieve a predictable and uniform whitening effect on their side teeth.[4]
Bleaching Comparison Facts
- 3 in-office applications of 38% Hydrogen Peroxide achieved the same result as 1 week of 10% carbamide peroxide nightly or 16 daily applications of 5.3% hydrogen peroxide on OTC whitening strips.[17]
- Attempting to use higher concentrations of bleaching solution to shorten the time required for tooth whitening makes no difference in the final outcome.[3] [4] [7]
- Attempting to use higher concentrations of bleaching solution can, however, increase tooth sensitivity and/or rebound (a reversal of the whitening effect) [18]
Common Sense Conclusions
In-office power bleaching works. Unfortunately, a significant part of the initial whitening effect is due to temporary tooth dehydration—which rapidly reverses as the teeth become wet again with saliva. The light used has been shown to provide no long-term enhancement to the whitening outcome. The procedure costs more, must be repeated more, and has a higher risk of tooth sensitivity than at-home tray techniques. Manufacturers even recommend the use of additional at-home tray procedures anyway.
Over-the-counter do-it-yourself bleaching works. Unfortunately, the lower concentration of bleach often takes much more time and many more treatment repetitions to achieve a desired result when compared to at-home tray techniques. The one-size-fits-all strips are more prone to gum sensitivity and may be more difficult for some patients to get a uniform whitening for their side teeth.
At-home tray bleaching works best. It creates the longest-lasting tooth whitening results in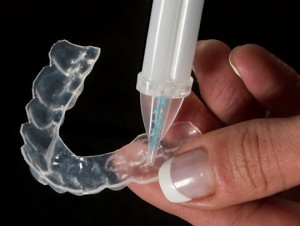 the least amount of time. Although some patients experience tooth sensitivity during treatment, the custom-fitted tray, solution (carbamide peroxide), and lower concentration of bleach (~10%) all reduce that possibility.
the least amount of time. Although some patients experience tooth sensitivity during treatment, the custom-fitted tray, solution (carbamide peroxide), and lower concentration of bleach (~10%) all reduce that possibility.
It would be great if tooth whitening worked perfectly for every tooth with every patient. As you might expect, however, some teeth don’t respond as well as others. We will investigate how to predict the outcome in our next post: “Whiter Teeth! (Part 5)”. Stay tuned.
Copyright © 2013 Stephen R. Snow, DDS
(I know you count on me to evaluate scientific study on your behalf and to apply relevant advances and discoveries in the recommendations we make and the treatment we deliver at Snow Dental Care. If you still want to dig a little deeper on your own about tooth bleaching, I have included references—and even links, when possible—for the scientific facts included here so you can investigate more if you’d like.)
[2] Haywood VB. Frequently asked questions about bleaching. Compend. 2003;24:324-337.
[4] Haywood VB. The “bottom line” on bleaching 2008. Inside Dentistry. 2008;Feb:2-.5
[5] Matis BA. Tray whitening: what the evidence shows. Compend Contin Educ Dent. 2003;24(4A):354-362.
[6] Haywood VB. Tooth Whitening: Indications and outcomes of Nightguard Vital Bleaching. Hanover Park, Il: Quintessence Publishing Company Inc; 2007.
[7] Gottardi MS, Brackett MG, Haywood VB. Number of in-office light-activated bleaching treatments needed to achieve patient satisfaction. Quintessence Int.2006;37(2):115-120.
[8] Browning WD, Swift EJ. Critical appraisal: comparison of the effectiveness and safety of carbamide peroxide whitening agents at different concentrations. J Esthet Restor Dent. 2007;19(5):289-296.
[9] Christensen GJ. Bleaching teeth: which way is best? J Esthet Dent. 2003;15(3):137-140.
[10] Mokhlis GR, Matis BA, Cochran MA, Eckert GJ. A clinical evaluation of carbamide peroxide and hydrogen peroxide whitening agents during daytime use. J Am Dent Assoc. 2000;131(9):1269-1277.
[11] Browning WD, Blalock JS, Frazier KB, et al. Duration and timing of sensitivity related to bleaching. J Esthet Restor Dent. 2007;19(5):256-264.
[13] Hein DK, Ploeger BJ, Wagstaff, et al. In-office vital tooth bleaching: what do lights add? Compend Contin Educ Dent 2003;24:340–52.
[14] Jones AH, Diaz-Arnold AM, Vargas MA, Cobb DS. Colorimetric assessment of laser and home bleaching techniques. J Esthet Dent 1999; 11:87–94.
[15] Papathanasiou A, Kastali S, Perry R, Kugel G. Clinical evaluation of a 35% hydrogen peroxide in-office whitening system. Compendium 2002; 23:335–346.
[16] Gottardi MS, Brackett MG, Haywood VB. Number of in-office light-activated bleaching treatments needed to achieve patient satisfaction. Quintessence Int 2006;37:115–20.
[17] Auschill TM, Hellwig E, Schmidate S, et al. Efficacy, side-effects, and patients’ acceptance of different bleaching techniques (OTC, in-office, at-home). Operative Dent. 2005;30(2):155-163.

